Principle 17 zet zich in voor transzorg op maat in Nederland. Zorg indien je die nodig hebt, wanneer je die nodig hebt, zoals je die nodig hebt.
Wij geven informatie over je rechten als trans zorgvrager, doen onderzoek naar de transzorg en staan zo nodig op de barricaden. In 2023 hebben wij een alternatieve zorgvisie gepubliceerd, die voldoet aan de mensenrechten van trans zorgvragers.
» Wie zijn wij? | » Wat doen wij?
Laatste nieuws
- Belangrijke bloedwaarden als je hormonen gebruikt

- Hebben trans tieners recht op hun lichaam?

- Nederland discrimineert transgender personen
- Wat heb jij nodig aan zorg? En kun je dat krijgen?

- OP 30 SEPTEMBER DEMONSTREERT TRANS ZORG NU 1020 MINUTEN VOOR BETERE TRANSITIE ZORG

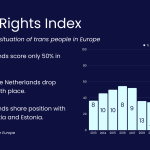
- Nederland doet het niet goed met LHBTI-rechten



